Two factors have been affecting the healthcare industry over the past several years. First, the passage of the Affordable Care Act (ACA) highlights the already intense focus on quality-based payments for patient care. Instead of paying physicians and hospitals for volume of care, they are now measured on outcomes: tracking errors, patient safety, and mortality and morbidity and paid accordingly.
Second, there is the need for relevant continuing education to respond to the changing healthcare environment and expectations.
The continuing education model is now expected to link a healthcare professional’s performance with a goal to improve patient outcomes. While evidence exists that continuing medical education (CME) is effective, the changing landscape now requires a more tangible link to show improved physician performance as documented in the section “Does continuing medical education (CME) improve physician performance and patient health outcomes?” in Effectiveness of Continuing Medical Education: Updated Synthesis of Systematic Reviews, by Dr. Ronald Cervero and Dr. Julie K. Gaines.
Driven by both external and internal factors, the healthcare industry is now leveraging the aspects of online learning that make it a priceless tool for improving workflow and processes, as well as for identifying gaps and performance improvement opportunities.
eLearning stimulates change in practice and performance
There is an abundant array of articles outlining how online learning can and should change performance on the job. But nowhere is that more critical than in the healthcare setting. Effecting change in performance in healthcare can mean the difference between life and death, or at the very least, can help prevent avoidable errors.
This shift from live meetings for continuing education to online or a combination of the two (blended learning) helps move education from an exercise solely in knowledge acquisition to one of simulated and actual performance improvement and behavioral change.
With eLearning, healthcare providers can engage in continuing education “with context.” eLearning supports the addition of interactive elements that foster behavior or process change, such as simulation techniques, case-based or clinical case scenarios, and pre- and post-testing to identify and close knowledge gaps.
With the post-learning activities, hospitals and healthcare systems can then measure performance improvement and track outcomes on an ongoing basis to ensure new processes and procedures not only take hold, but also remain in force for long-term gain.
Online education helps change new-mother experience
In 1991, the Baby-Friendly Hospital Initiative (BFHI) was launched by the World Health Organization (WHO) and UNICEF, and kicked off a global effort to implement practices that protect, promote, and support breastfeeding. The US-based Baby-Friendly Hospital Initiative encourages and recognizes hospitals and birthing centers that offer an “optimal level of care for infant feeding and mother/baby bonding.”
According to the CDC, although from 2000 – 2008, the percentage of women who initiated breastfeeding increased from 47.4 percent to 58.9 percent for blacks, and 71.8 percent to 75.2 percent for whites, only 23.4 percent met the recommended breastfeeding duration of 12 months, indicating women may need more support to continue breastfeeding.
The Virginia Department of Health (VDH), as part of a statewide initiative, sought to foster the adoption of exclusive breastfeeding and to encourage hospitals and maternity centers to participate in this program through the development of the Virginia Maternity Center Breastfeeding-Friendly Designation (VA MCBFD) Program. Nurses and pediatricians needed to be well informed about the evidence supporting breastfeeding so they could implement standardized approaches to support and coordinate the care of mother and baby.
Online education helps support coordinated, multi-disciplinary care
For new, and especially first-time mothers, the first two days are critical for easing both baby and mother into breastfeeding. VDH recognized the importance of educating caregivers on breastfeeding and developed content, but they needed a platform and technologies. VDH collaborated with the University of Virginia Office of CME to create a multi-dimensional learning platform that provides a comprehensive educational experience for nurses and pediatricians.
The Breastfeeding Consortium project (http://bfconsortium.org ) is led by the UVA School of Medicine in collaboration with HIT Global, Telligen, and Scitent. This unique platform promotes breastfeeding training through eLearning, performance improvement, and a registry tracking and quality assurance system to educate and inspire healthcare providers to work better as a team to improve the success rate for breastfeeding.
The first part of this effort involved developing an online breastfeeding training course with Scitent. The aim was to design a flexible online course that would support the entire “New Mom” team: from the nurse and lactation consultant to the pediatrician and compliance team (Figure 1).

Figure 1: An online breastfeeding training course supports the “New Mom” team: from the nurse and lactation consultant to the pediatrician and compliance team.
The educational content speaks to all team members and includes information on history, culture, and breastfeeding challenges, as well as case scenarios and information on caring for infants with special needs. However, the content is also designed to address the unique role of each team member while also showing how roles interconnect. In the case of the physician, essential clinical content geared toward the pediatrician (specialist) is offered through an online performance improvement module created by HIT-Global that awards Maintenance of Certification (MOC) Part IV to pediatricians (Figures 2 and 3).

Figure 2: eLearning in healthcare is aided by the inclusion of case studies and case-based scenarios so that professionals learn what to do, in a real-world context.
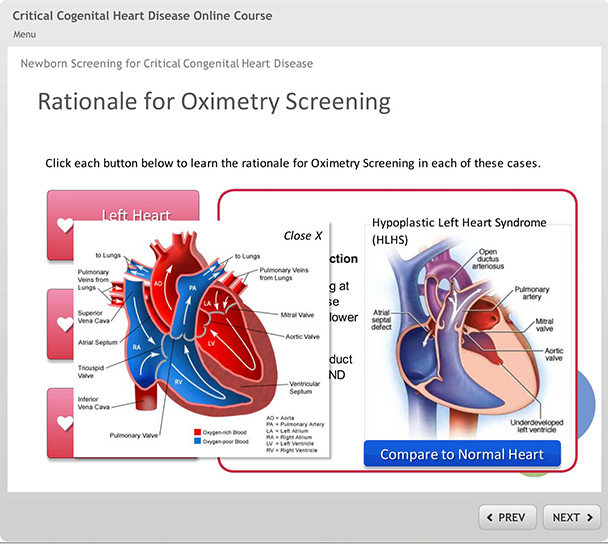
Figure 3: A newborn screening course focuses on critical congenital heart disease (CCHD) and is delivered in two configurations – one for nurses, and one for physicians who have to interpret the results and enact follow-up procedures for a failed screen.
In addition to supporting cross-team education needs, the Breastfeeding eLearning course was designed to support healthcare staff in other ways, including:
- Use of multimedia and video to highlight do’s and don’ts and how to recognize key techniques, such as, “Is the baby latching on correctly?”
- Inclusion of case studies and case-based reviews to learn what to do in a real-world context
- Ability to stop and start learning so busy providers can pick up where they left off and drive the pace of learning
- Learning that can be blended with in-person and on-site training
- Integration with an individual Performance Improvement Course and Hospital Chart Auditing tool
The second piece of this effort is performance improvement. The performance improvement aspect was developed initially for individual physicians wanting to improve their knowledge and support of breastfeeding. It was later expanded so hospitals could enter multi-physician or practitioner baseline data to identify gaps in practice, develop educational efforts to address these gaps, and then document a sustained change in practice.
The final element in the platform is the patient registry. Hospitals can voluntarily utilize a web-based tool to capture clinical data in real-time, and compare variations in a provider’s performance against breastfeeding clinical guidelines.
This immediate feedback highlights gaps in care, or variations that are not consistent with exclusive breastfeeding. The availability of resources and access to the learning platform helps maintain a culture of continued improvement towards meeting the current standards of care.
eLearning reminds providers of the patient experience
Another UVA Health System initiative, Newborn Screening Education http://www.newbornscreeningeducation.org/, utilizes online learning modules to educate the newborn care team (nurse and pediatrician) on priorities for newborn care, while also introducing a differentiated approach for each provider based on their role.
The Newborn Screening Education Project is a joint venture between the VDH, the University of Virginia Office of Continuing Medical Education and Scitent to provide healthcare professionals and institutions nationwide with certified continuing medical education opportunities to ensure that every well newborn is accurately screened prior to discharge from the hospital.
One learning course focuses on screening for critical congenital heart disease (CCHD) and is delivered in two configurations—one for nurses, and one for physicians who have to interpret the results and enact follow-up procedures for a failed screen. Further, nurses are presented with an additional online module—A Provider’s Guide to What Parents Need to Know About Critical Congenital Heart Disease—which helps nurses communicate with parents and address their concerns about why their newborn needs the testing, and the need for follow-up if the baby experiences a failed screen.
This type of differentiated online learning leverages common goals while using multiple learning approaches to reinforce consistent patient care priorities that may vary, depending on a provider’s relationship with the newborn or mother. While both the physician and nurse need the same data to make informed decisions on the infant’s cardiac function, they each have different roles in implementing a plan of action.
Online learning adapts to providers’ workflow
While live meetings in healthcare will continue, as the format can provide an important way to connect and network with others in their field, a continued increase in online learning is an effective strategy for receiving time-sensitive and focused learning that can impact performance.
eLearning delivers consistent cross-team learning, allows providers to consume engaging content in short bursts (between rounds or at the end of a shift), presents case-based scenarios and real-time testing to reinforce learning, and allows providers to integrate learning with performance improvement initiatives.
In an industry where knowledge has the power to heal, online learning will continue to grow and evolve to meet rapid advances in healthcare and delivery.


